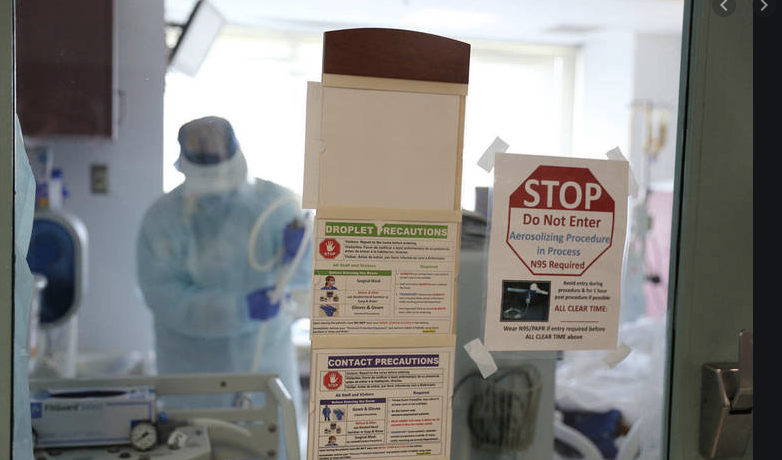
Today we caught up with Sam, a nurse working in a cardiac ICU unit at a medium-sized private hospital in Newark NJ. In Sam’s workplace, a nurse was recently suspended for organizing a gofundme page to raise money for more PPE equipment. Sam’s co-workers believe that she was targeted because management believed that she was agitating to start a union. Due to these recent events, Sam asked that we use gender-neutral language to minimize the risk of being identified by management.
Sam was getting ready to go in for their usual 12-hour shift. We talked about Sam’s fears and worries going to work and how the coronavirus has impacted their daily life and workplace.
Can you tell us a little bit about what you do as a nurse?
I am a nurse in a mixed medical-surgical ICU/cardiac ICU unit where we handle mostly cardiac ICU patients. It is my responsibility to monitor patients, independently assess how they are doing, which way their health is trending and make interventions as part of our care team which includes respiratory therapists, nutritionists and other health care practitioners to get our patients healthy. As a medical surgical ICU, we generally take sick people who require closer monitoring than a telemetry floor (where they do regularly cardiac monitoring). We also have a heart transplant team and that’s we are well known for. We manage and care for a lot of patients who are either being worked up for a heart transplant or have already had heart transplants and when they have difficulties resulting from it, they come back to us. We clean them, we turn them, get them food, take care of their respiratory status. A lot of our patients are intubated or sedated so they can’t do anything on their own and generally rely on us to take care of them.
I’m finding that many people aren’t familiar with some of the terminology. Patients are intubated, meaning they have a breathing tube inserted through their mouth, down their trachea, and to their lungs. The tube is attached to a ventilator that forcibly pushes oxygen at set concentrations, rates, and pressure into their lungs. The uncomfortable and even painful nature of this requires many patients to be paralyzed for the insertion of the tube, and then chemically sedated for the duration that the tube is in.
I started in the ICU because I wanted to be in a more contained and controlled environment where I felt I had a stronger sense of what was going on in my patients. I wanted to deal with as little chaos as possible while working in a hospital. I was also eager to learn more about critically ill patients and the work that goes into getting them better again. I was willing to trade the higher volume of patients in my previous positions for lower volume and higher acuity.
Well is the ICU less chaotic now especially with the COVID-19 outbreak?
Well before anything of this was happening, I don’t want to say we were business as usual. There were some happenings for sure. For instance, there was an article on ProPublica about our unit’s treatment of a patient and the heart transplant unit was certainly under fire. But this didn’t concern the nurses because it had nothing to do with us. It was mainly a problem stemming from the doctors and the administrators. The nurses were not mentioned negatively in the expose at all. But I guess I want to say that things were normal–as much as things can be working in a hospital. We had some problems that affected nurses like we are sometimes understaffed, feeling like we had to deal with occasional medical shortages, etc. These are issues that pop out every now and then but again they are not out of the ordinary for us.
But now the COVID-19 has made everyone tense and fearful. It hangs over us nurses like a cloud. Most of our conversations are about the coronavirus and Covid-19. It has made everyone more scared of their own health to begin with which wasn’t a concern while working. You felt generally safe but now there are constant struggles to get the necessary PPE (Personal Protective Equipment) we need to work.
It seems like personal protective equipment is even more important in an ICU.
Oh, for sure. We have patients who are being treated for many different types of contagious organisms, which require different levels of precaution and PPE. In the old days prior to the COVID-19 outbreak, we just wore scrubs for our general patients but now that’s harder to do because of this virus.
Where I work besides our regular patients, we also take care of those that are on contact precautions because they have an infectious organism. MRSA (Methycillin-resisitant staphylocaccus aureus) and ESBL (Extended Spectrum Beta-Lactamase) are two common organisms that spread through contact, which requires us to wear a disposable gown and gloves in addition to our standard precautions of hand washing. Above that you have patients that have droplets precautions meaning they have an infectious disease that can spread through droplets. So, after a patient coughs these droplets are there and this is where the 6 foot rule comes from. Then there is airborne isolation and that’s for when these things can just hang in the air. For this we use negative pressure rooms which we have very few. There are three levels from contact to droplet to airborne.
I am still not clear on whether the novel Coronavirus is spread by airborne or droplets. We are not clear on whether our clothes are safe. We hear bits of stories about the virus living on people’s hair or on different surfaces. The idea of there being an entirely new virus that is killing people is very scary to us, which is why we want to be protected. I am personally wearing a Tyvek suit, an N95 respirator, a face shield, as well as the disposable gown and gloves.
That’s insane. Can you tell us more about your access to this equipment? The media is certainly highlighting shortages. How true is this for your unit?
Well, I had to buy the Tyvek suit myself if that gives you any indication. And there are multiple kinds of shortages. Other than the testing, there is the lack of personal protective equipment which people have called attention to. Two weeks ago when I went into work they had a sign-up sheet and every worker was handed a single surgical mask and paper bag along with a note that read: “Here is a mask. You can wear it when you interact with patients and due to shortages you have to use it as much as possible and store it in this paper bag after your shift.” Now you have to understand that before Covid-19 we had a bunch of these masks and we used them for single patient interaction. Especially for patients with special cautions in place. This means before you enter a patient’s room, you put it on, use it and throw it away and wash your hands. Now they are telling us to hold it not only for entire shift but subsequent shifts. So I work 12-hour shifts for three days and I’m expected to have one mask for all these hours. But these masks, they are not made to be durable like that, and they lose their effectiveness when used in this way. So that was about two weeks ago.
Last week we had been given paper scrubs to put over our regular clothes and then we placed our plastic gowns over it. Right now, we are out of paper scrubs. So, this is why I bought the Tyvek suit because there are no paper scrubs and I want to cover every inch of skin that may be exposed.
So, equipment shortage is one and another shortage is the ICU beds. The COVID-19 patients are incredibly sick. They go over a cliff in terms of their health real quick and very seriously. They get sick fast and precipitously decline. The amount of beds that we have available is always a matter. Your typical respiratory patient may require for a week and be ventilator dependent for a week. These COVID-19 patients on the other hand, if they survive that long, though will need the beds for multiple weeks. They may also need dialysis because of things ling kidney failure, or blood transfusions or other interventions. Taking care of Covid-19 patients is very labor intensive.
Shortage of nurses is another. The media and Cuomo is saying that NYC will need 30,000 ventilators when they imagine it will peak in a few weeks. I am not sure they have enoughnurses and respiratory therapists for managing and operating them. You see medical/surgical nurses are not trained to use this equipment that we use in the ICU. They are not trained to deal with ventilator dependent patients. It’s not just equipment and beds, it’s also the labor that goes all into it.

Can you tell us a little bit about how the vents work and why not everyone is equipped to operate them?
Vents are complex machines that do far more than squeeze a bag of air into someone’s lungs. When we speak of someone who is intubated, in this case it means someone who is invasively (through the breathing tube) ventilated. The vent tries to push a volume of an air/oxygen mixture into the patient’s lungs at the lowest pressure it can. With our COVID patients and their viral pneumonia, the microscopic air sacks where oxygen exchange takes place fills with fluid and can collapse. The ventilators use something called PEEP to keep their small airways open. As COVID-19 patients progress from viral pneumonia to ARDS (acute respiratory distress syndrome), they require higher amounts of PEEP and higher concentrations of oxygen to meet their body’s demands. High levels of PEEP are risky because they can cause damage to the lung tissue, but may be required to keep our patients alive. The effectiveness of the ventilation is measured initially by the oxygen readouts on the monitors, but requires frequent arterial blood gas tests (blood samples taken from an artery instead of a vein) to get a true understanding of how much oxygen is really getting to a person’s circulatory system or how much carbon dioxide is getting expelled. With this information, frequent changes can be made in the ventilator to match its settings to the needs of the patient.
When I say that med/surg nurses are not trained to use vents or any of the many devices that are frequently found in an ICU, that is not to disparage their training or knowledge. But a patient that is intubated requires an ICU level of care and it’s simply not safe to have a med/surge nurse, who might already have 5 or 7 other patients, also provide care for a patient on a ventilator. A typical ICU nurse will have 2 patients, one might have 3 if you’re unlucky with staffing. Last week, every ICU nurse had 4 patients. Most, if not all, intubated, some receiving continuous dialysis also run by the same nurse. These are labor-intensive patients.
What is it like working with COVID-19 patients? Do you have a sense of how many Covid-19 patients you and other nurses are handling?
We haven’t lived through a pandemic of this sort. I was surprised how deadly the flu could be to some people. But these are generally older people but with COVID-19, I am also seeing some young people. We’ve done CPR on multiple people in their 20s and 30s already.
COVID-19 patients come in and they have been complaining about shortness of breath about week or two before hospitalization. When they come in we give them oxygen, we start with Hydroxychloroquine and Azithromycin and depending on what source you’re looking at may include Doxycycline, Zinc, Vitamin C, and others. We keep them prone meaning they lay on their stomach. Initially this seems help some for a little while but then they have these sudden declines that require intubation and ventilation.
So, President Trump has been making a lot of hay about a supposed miracle treatment for COVID-19. Anecdotally, these treatments may help some people. But the research is not conclusively pointing to it being effective at all. Our morgue is filled with the bodies of those who received this supposedly miracle drug cocktail. Many of them still decline and need extra oxygenation, which will require intubation and ventilation.
When this happens some of them are sedated and paralyzed and it’s still hard to oxygenate them. From that point a lot of them are still progressing into septicorgan failure. Soon their kidneys require dialysis. It seems a matter of time you have to do CPR on them. They go off that cliff real quick and little that we do seems to be changing that trajectory at all.
Anecdotally, Covid-19 patients do seem to be older, overweight and the ones that have preexisting cardiac and lung issues seem to be doing the worst.
We also have a bunch of patients who maybe were negative on their swab test. But they have elevated blood markers, and their chest CT and other signs and symptoms definitely show that they have the virus but the swab comes negative. This happens with regularity. It’s a false negative. From the standpoint of a health care provider this is maddening.
It’s hard for me to tell now many COVID-19 patients we have but I know that our COVID ICU is full. Because as soon as this started spreading, we opened a new COVID-19 unit and it’s now full. I do some shifts there. I divide my time between this and our regular ICU which is also filling up with COVID-19 patients. As people leave our regular cardiac ICU they are being replaced most often with COVID-19 patients.
As a nurse, what most worries you about everything right now?
That this is not going to end. We are hearing about flattening the curve, slowing down the rate of infections with isolation and self-quarantining but a lot of people’s hope are predicated on these and either a vaccine developed or the illness cycling out like influenza over the winter months.
I am not sure this is possible. For one, a vaccine might not be available for years if ever and two, there is no real evidence that this will wax and wane like seasonal flu. This beg the questions that people continue to be infectious and the disease is as deadly what will happen in a month or two when mayors and employers want people to go back to work to protect the economy. A lot of our elected officials didn’t expect to have to make these life and death calls. Their main job is to manage the markets and I feel eventually these market concerns are going to call them to task and they will feel the pressure to have people go back to work. And what will happen if people go back to work? This thing will once again spread like wildfire.
Recently, Propublica reported that your co-worker, an ICU nurse, was suspended for starting a gofundme page to raise money to buy protective supplies to distribute to colleagues. Do you believe that there is something more to this story than what was reported?
That story is incomplete. Propublica writes “The hospital told ProPublica in a statement that Matievskaya’s suspension ended Monday. “No employee is allowed to distribute unauthorized medical supplies within the hospital,” the statement said. “The nurse in question was temporarily suspended for inappropriately distributing unauthorized medical supplies, against this policy.” But this is an incorrect post-hoc justification of the nurse’s suspension. I do not doubt that there is a line somewhere in some policy document against distributing unauthorized equipment, but she was suspended for shining an unflattering light on the hospital and over fears she was agitating staff towards unionization. It seems, that even in the midst of a global pandemic, the old rules and old fears are still motivating the people in the ways we’ve always known them to.
How has this incident and the COVID-19 pandemic in general changed how you view your job?
I feel like even before the COVID-19 outbreak, I knew the American health care system was awful and inhumanely focused on profits and on doing things besides keeping people healthy. We were good for those that have access to healthcare but for everyone else no. We were just doing the minimum possible and trying to get them to not come back. On one level this virus is exposing the myriad weaknesses in our health care system. Just like those around the world. Some of our weaknesses have been caused by profit motive like the complete lack of stockpiling of resources that would be needed if things got bad. They are talking about how in a year they think that health insurance premiums may go up by as much as 40%. I am hoping that will be enough to understand to cause the need for Medicare for All which has been important for me as a nurse. The idea that you and your family’s health insurance has to be tied to you working and being employed is absurd. And in a pandemic when people can’t work, tying health insurance to work is a bad idea for society. Your personal health is dependent on the health of people around you. You just can’t buy your way to better healthcare. Not when there is an infectious disease around you.
Presidential candidate Joe Biden has multiple times now said that policies like Medicare 4 All would not make this virus better. He’s both wrong and right. The way we allocate healthcare resources in this country would not make a dangerous virus any less virulent. But if you are thinking about all the families of the deceased as well as those who survived being critically ill- they may disagree when they receive a 6-figure bill in the mail. Those who survive and are now looking at possible ongoing respiratory issues or rehab may think otherwise as well.
As a nurse, I feel like people are right to get upset about the hoarding that we have to deal with and how little equipment we have to address this pandemic. We now have to jump through these hoops wondering what could happen when we don’t get it at all. I imagine that will come pretty soon. Nurses are worried. We are sometimes told we don’t need a whole body get up. Just protect your face and that will be enough. But they have no idea how that will affect us and our families. You want to be able to do your job but you also want to go home and be safe after you are done. I don’t know what I’d do. I’d like to think I would keep trying to help my patients. I know some people said they would quit if the hospitals don’t protect us. When we get to that stage individuals will have to choose about what they feel comfortable with. Also it doesn’t help that our hospital nurses are not unionized. Honestly, I don’t know what’s going to happen.
How has your work-life routine changed because of this? I imagine your loved ones are worried about you.
As soon as I get to my apartment door, I take all the clothes, put them in a hamper we have placed outside and I head straight into the shower. After I shower, I disinfect all the things I had in my pockets: phones, pen, keys things like that. I try to avoid bringing anything home to my apartment. My partner and I don’t go out to bars. I haven’t seen my friends face to face for a few weeks now. I had to cancel a few trips. This is all so bad and I am concerned that it may not really get better. And on top of this, people are being told to go back to work because of “the economy.”
Yea, what do you think about that?
I wish we can come to a new understanding about people’s relationship to work and labor and I wish I could wave a wand and show that we need a long-term approach. We have to change the way we live, and it can’t just be for the next three weeks. I wish I could get them to all vote for Bernie Sanders! (laughter). Trump is gonna be on that stage rambling nonsense. But his approval ratings have never been higher. We don’t deserve Bernie, we are all awful. Bad times. I didn’t want to live during a pandemic; it turns out that it sucks. It’s awful.
Amidst all of this, what message would you want to relay to our readers?
For one I wish people would stay home. I sometimes wish that when I see people hanging out, I wish they could be a fly in the wall of our ICU. Our hospital is completely on lockdown unless someone is giving birth or is dying. I have patients who are critically ill, intubated, sedated and paralyzed and on top of that I have to tell their families, no you can’t come see your loved ones everyone is infectious here. And until the moment they die they can’t see their family. When they die they die quickly. We sometimes may anticipate it and we contact their families to come in. But even than they can only come in one at a time and look through a window at their loved ones for just a few minutes. It’s dire in a way that’s I can’t just describe in words.
Our relationship to work and labor has to change. If your job is answering phones and typing on a computer, maybe you don’t need to be there. Maybe we need a long-term look into how we can change our lives so that we can mitigate the effects of this pandemic in a longer-term fashion not just for the next three weeks. Additionally, what we call low-wage work is essential work. You know bankers and financial analysts they stay home and nothing changes. Those that do low skill work, which is insulting to call it that, they are the ones that can bring this economy to a halt when they stay home.
***
We are looking for testimonials from everyday people about workplace safety, unemployment and housing issues, struggles with paying bills and taking care of their loved ones, as well as any acts of solidarity and collective action in these very difficult times. We want to hear from you! If you have a story that you want to share with us, please email the editor at editor@hardcrackers.wqzzauofih-ypj689jde4l2.p.temp-site.link